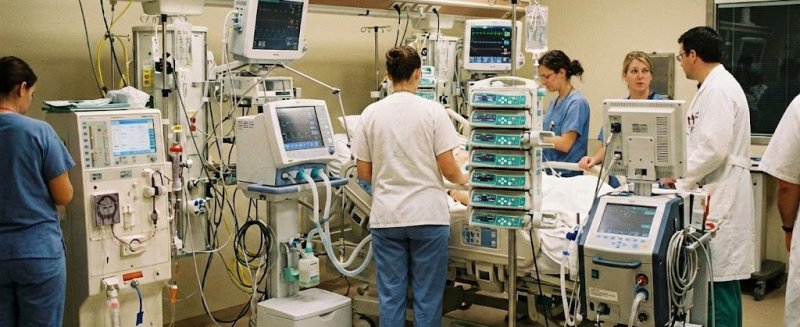
Medical assistive machines are categorized according to their clinical purpose, operational mechanics, and integration level within hospital infrastructures. This classification helps determine the role, impact potential, and functional boundaries of each device.
Diagnostic support machines provide high-resolution imaging, physiological measurement, and algorithmic analysis that enable rapid and accurate detection of medical conditions. Systems such as X-ray, ultrasound, CT, and MRI generate detailed anatomical views, while ECG modules and blood-pressure monitors capture real-time electrical and hemodynamic activity.
In well-equipped institutions, advanced imaging modules can process more than 20,000 data samples per second, resulting in highly detailed diagnostic insights. AI-supported analysis engines further refine these outputs by identifying anomalies, prioritizing risk patterns, and suggesting data-driven interpretations. These mechanisms increase diagnostic precision and facilitate early intervention for critical conditions.
- High-frequency sensor arrays
- Multi-layer image processors
- Adaptive reconstruction algorithms
- Automated pattern-recognition modules
The combined effect of these technologies significantly reduces misinterpretation rates and accelerates physician workflow.
Treatment support machines control medication delivery, support respiratory function, and assist in surgical precision. Smart infusion pumps eliminate dosing variability by regulating flow rates with micro-scale accuracy. Mechanical ventilators ensure stable gas exchange dynamics for patients experiencing respiratory failure.
Robotic surgical systems contribute remarkable stability and accuracy through articulated arms, enhanced visualization channels, and latency-free control modules. Healthcare institutions utilizing robotic platforms report up to 15% shorter postoperative recovery times, demonstrating the clinical value of technologically enhanced interventions.
Rehabilitation systems focus on restoring motor functions, strengthening neuromuscular coordination, and promoting controlled mobility in patients recovering from neurological or orthopedic conditions. Robotic gait trainers, balance simulation platforms, and targeted muscle stimulation devices form the core of this category.
The cyclic repetition of optimized movement patterns strengthens neuroplastic pathways, supporting measurable functional gains. Statistical evaluations from specialized rehabilitation centers show that structured robotic rehabilitation programs reduce the average recovery timeline by approximately 10%.
Medical assistive machines operate through multi-layered technical architectures composed of sensors, processors, software protocols, and user interfaces. This layered structure governs how data is captured, interpreted, and translated into actionable clinical feedback.
- Sensor Layer:<span> </span>Captures biometric, physiological, or mechanical input.
- Processing Layer:<span> </span>Filters, analyzes, and validates collected data.
- Output Layer:<span> </span>Generates visual, auditory, or electronic clinical feedback.
- Safety Layer:<span> </span>Continuously monitors system boundaries and triggers protective modes when anomalies are detected.
Professional-grade systems can process more than 40,000 data points per operational cycle, enabling precise decision support under demanding clinical workloads.
Medical assistive machines account for nearly 40% of equipment portfolios in modern hospitals. Their variety enables consistent monitoring, standardized intervention, and reliable care delivery across different clinical departments.
Vital-sign monitoring systems measure heart rate, oxygen saturation, blood pressure, respiration, and temperature with second-by-second accuracy. These systems are indispensable in intensive care units, emergency departments, and postoperative recovery rooms.
Integrated alarm modules allow clinical teams to respond rapidly to unexpected physiological changes. Data logs generated by these systems form essential input for both retrospective analysis and predictive modeling.
Medication management machines regulate drug administration by controlling dosage, timing, and infusion parameters. Intelligent pumps incorporate error-prevention algorithms, dose-limit protections, and automated shutdown functions.
Hospitals implementing these systems consistently report up to 50% reduction in dosing errors, making them one of the most impactful safety-focused innovations in medication delivery.
Sterilization systems safeguard surgical environments by eliminating microorganisms through high-pressure steam above 120°C, UV-C light technology, and advanced filtration methods.
Clinical facilities with modern sterilization infrastructure observe surgical-site infection rates approximately 12% lower than facilities using outdated systems, demonstrating the preventive value of high-grade sterilization machines.
Artificial intelligence substantially enhances the performance, reliability, and predictive capability of medical assistive machines. Machine-learning models analyze data patterns, detect anomalies, predict equipment failures, and assist clinicians with risk-based decision support.
- Early anomaly detection
- Predictive maintenance modeling
- Real-time classification of risk indicators
- Automated triage suggestion
- Workflow optimization
Devices equipped with AI modules record an 18% reduction in mechanical or operational failures, improving long-term device sustainability.
Medical assistive machines must comply with strict international safety protocols to ensure operational reliability. Standards such as ISO 13485, IEC 60601, and biocompatibility frameworks regulate design principles, material safety, electromagnetic compatibility, and performance stability.
- Multi-phase validation testing
- Redundant fail-safe mechanisms
- Thermal and electrical overload protection
- Electromagnetic shielding systems
- Biocompatible material compliance
Adherence to these standards ensures high reliability in intense clinical environments where malfunction risks must remain exceptionally low.
Strategic placement of machines improves operational efficiency, reduces clinician travel time, and enhances patient safety. Positioning is determined by human-traffic density, departmental workflows, and required access speed.
| Department |
Purpose |
| Intensive Care |
Continuous physiological monitoring |
| Emergency Unit |
Rapid diagnostic and stabilization tools |
| Operating Room |
Imaging, sterilization, robotic support |
| Rehabilitation |
Mobility training and neuromuscular activation |
Correct placement also reduces bottlenecks and ensures uninterrupted operation during peak clinical hours.
Medical assistive machines reduce manual workload, optimize task distribution, and provide clinicians with richer and more consistent data. By automating routine tasks, these devices allow medical professionals to concentrate on complex decision-making and patient-centered care.
- Up to 25% reduction in clinical workload
- Increased documentation accuracy
- Faster patient throughput
- More consistent risk evaluation
- Improved multidisciplinary coordination
These shifts contribute to a more resilient healthcare ecosystem in which professionals can operate with greater precision and lower cognitive fatigue.
Home-use medical assistive machines support chronic disease management outside hospital environments. Devices such as portable ECG systems, digital blood-pressure monitors, nebulizers, and smart glucose meters enable accurate self-monitoring and remote clinical supervision.
Market analyses reveal an approximate 11% growth in the home-care equipment sector within the past year, driven by aging populations and increased demand for decentralized care.
As clinical technology evolves, medical assistive machines are expected to become more autonomous, more interconnected, and more predictive. Integration with wearable devices, cloud-based analytics, and hybrid hospital–home monitoring platforms will redefine the boundaries of patient care.
- Fully autonomous monitoring ecosystems
- AI-driven predictive diagnostics
- Robotic rehabilitation with adaptive feedback loops
- Integrated bio-sensor networks
- Hybrid telemedicine-assisted treatment channels
Forecasts suggest that by 2030, approximately 60% of hospital-based devices will incorporate AI-enabled components, underscoring the long-term shift toward intelligent healthcare automation.